Age-Related Macular Degeneration (AMD) is a disease of abrupt origin and is a leading cause of vision loss in older adults. The common cause of AMD is the gradual degeneration of the macula, the part of retina of the eye that provides a sharp, central vision. AMD advances rather slowly and vision loss does not occur for a prolonged period in some individuals. In others, a faster progress of the AMD in the eye is noticed that may lead to loss of vision in one or both the eyes. AMD is age related; people older than 50 and the risk increases with age. Other risk factors for macular degeneration are: Smoking, race, family history, obesity, sleep apnoea, cortisone medication, trauma, diabetes, etc. Age related macular degeneration is of two types, wet AMD and dry AMD. Both types of AMD can advance and cause severe vision loss. In wet AMD vision loss is due to growth of abnormal blood vessels. In dry AMD gradual changes occur in eyes leads to problems in central vision.
Age related macular degeneration (AMD) starts as a typical yellow deposit in macula. Symptoms of macular degeneration include blurry areas in the centre of vision; straight lines appear to be distorted, diminished colour perception etc. Macular degeneration can make it difficult to read or recognise face as age progresses.
Treatment: There is no absolute cure, but AMD treatments may prevent severe vision loss or slow down the progression of the disease. Non-drug interventions: Macular degeneration study suggests, vitamins (carotenoids, lutein and zeaxanthin), consuming omega-3 fatty acids, low glycemic index foods helps in reducing AMD progression. Laser therapy, photodynamic therapies are used in severe cases. Anti-VEGF agents, injected directly into the vitreous humor of the eye can cause regression of the abnormal blood vessels and improve vision.
Retinal Detachment
The retinal detachment is a retinal disorder in which the retina or the retinal nerve tissue peels away from the underlying layer is known as retinal detachment. Due to the detached retinal tissue, the retina loses its functional capacity and eventually causes a sudden and severe loss of vision, and if not treated properly it leads to ultimate blindness, shrinking and disfiguring of the eye. Most common cause of retinal detachment results from the formation of a hole in the retina. The vitreous fluid, a jelly like substance filling the eyeball, passes through this hole behind the retina and detaches it. Another form of retinal detachment that occurs due to diabetes or other retinal diseases is called tractional retinal detachment. Here the retina is pulled up by the contraction of extensive membranes formed on the retina. The central retinal occlusion and branch retinal occlusion cause vascular haemorrhage. The severe cases of retinal vein occlusion cause neovascularisation which eventually leads to retinal detachment. Central retinal artery occlusion is also associated with chronic retinal detachment. The risk factors for retinal detachment include the presence of high degrees of myopia, injury to the eye, occurrence of retinal detachment in the fellow eye, occurrence of retinal detachment in blood relatives, cataract surgery etc. Retinal detachments occur most commonly in younger adults (age 25 to 50) who are highly myopic and in older people post cataract surgery. The symptoms for retinal detachment include heaviness in the eye, sudden increase in floaters, photopsia, shadow in the peripheral vision which progress to central vision and straight lines appear to be curved.
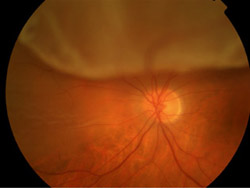
Retinal detachment treatment
A retinal specialist would be the best person to consult in case of retinal detachment and other disease like macular degeneration. A simple retinal treatment procedure using laser or Cryopexy procedure is used in a retinal tear without a detachment. Retinal detachment operations are urgent to settle the retina. Surgery for retinal detachment includes retinal surgery, vitreo-Retinal Surgery, scleral buckling surgery, or pneumatic retinopexy. They are selected according to the severity of the case and other factors by the retinal surgeon. In some cases, owing to the formation of membranes on the retina, re-detachment may occur (called Proliferative Vitreo Retinopathy). Recovery with retinal surgery is seen for the first time itself in 85% of patients. Visual clarity may not be clear as before especially in macular retinal detachment.